Home > To reconstruct an auricle that will not melt
Microtia surgery is a special surgery involving costal cartilage graft.
Nobody wants the reconstructed auricle contracted and deformed over time like 5 years or 10 years after the surgery.
For 6 months after the 1st-stage surgery of costal cartilage graft and before the 2nd stage surgery of auricular projection, grafted costal cartilage cells are alive thanks to nutritious body fluid from all around the reconstructed auricle.
However, right after separating the posterior auricle from the temporal region of head at the auricular projection surgery, the body fluid / blood circulation can be obtained from the anterior auricle only and the body fluid / blood circulation around the grafted costal cartilage remains reduced. The conventional Tanzer or Brent method utilizes skin graft only on the back of the separated auricle, which results in ear projected with wrong degrees as well as the post-operative shrinkage of the grafted skin, the tension from which could also generate bad effects even on the front side of the reconstructed auricle and its shape.
Reduced blood circulation described above could not make the grafted costal cartilage cells survive, which might be resorbed over time like 5 years or 10 years after the surgery. You can see some cases of the secondary auricular reconstruction performed in this clinic at the website of Nagata Microtia and Reconstructive Plastic Surgery Clinic, Secondary auricular reconstruction #1, Secondary auricular reconstruction #2 and Secondary auricular reconstruction #3, where the patients had previously received an auricular reconstruction with Tanzer method at another institution and then the grafted costal cartilage had been contracted and deformed unfavorably due to the resorption. The photos of preoperative appearances show how serious conditions could be brought by the resorption of the grafted costal cartilage.
Then, what kind of surgery is required to project the reconstructed auricle with correct angle and not to cause the resorption of the grafted costal cartilage? The answer is 1) to separate the posterior auricle from the temporal region of head, 2) to create a costal cartilage block of 14 mm thickness and put it on the back of the auricle between the auricle and the temporal region of head as a support to project the auricle with normal projection angle of 30 degrees, and 3) to cover the grafted costal cartilage and the entire back of the auricle with TPF (temporoparietal fascia) or “a membrane with the most abundant blood circulation including superficial temporal artery” elevated from the temporal region of head to make the costal cartilage cells alive.
The above mentioned method does not cause the post-operative shrinkage of the grafted skin as its feature.
As the result, the resorption of the grafted costal cartilage does not occur because the body fluid / blood circulation from the posterior reconstructed auricle can be further enhanced. Between 1992 and 1993, five (5) papers including this method and the principle theory were submitted to and posted on the journal of the American Society of Plastic Surgeons (ASPS) as Nagata method. See the publications at the website of Nagata Microtia and Reconstructive Plastic Surgery Clinic. Thereafter Nagata method spreads gradually across the world and appears in the textbook published by the ASPS.
Also, the author has attended the Plastic Surgery The Meeting, which is held by ASPS every autumn, has served as an instructor of the microtia instructional course and has given a lecture / guidance. However, the surgical technique itself is very difficult and thus surgeons need a long period of training of this field.
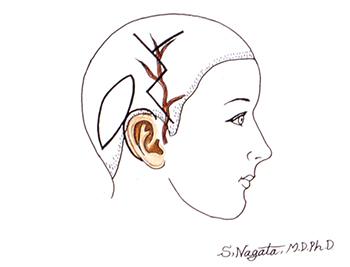
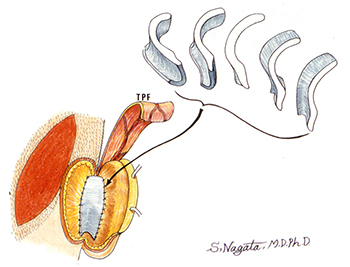
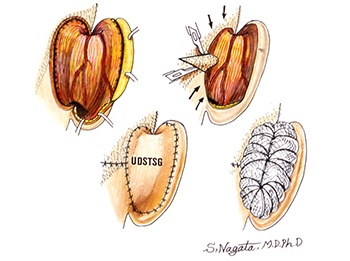
Though the morphological shape is maintained for the first 1 year after the surgery with three-dimensional costal cartilage graft utilizing Nagata method for the first stage but with a simplified method of auricular projection for the second stage not utilizing TPF to avoid complex and time-consuming surgery would result in melting of the reconstructed auricle due to the resorption of the grafted costal cartilage 10 years after the surgery and the patients might fall into serious conditions with the reconstructed auricle contracted and deformed.
I believe that it is surgeons’ mission to continue the training to reconstruct the auricle with good blood circulation in spite of difficulties.



